Pelvic Floor Dysfunction (PFD)
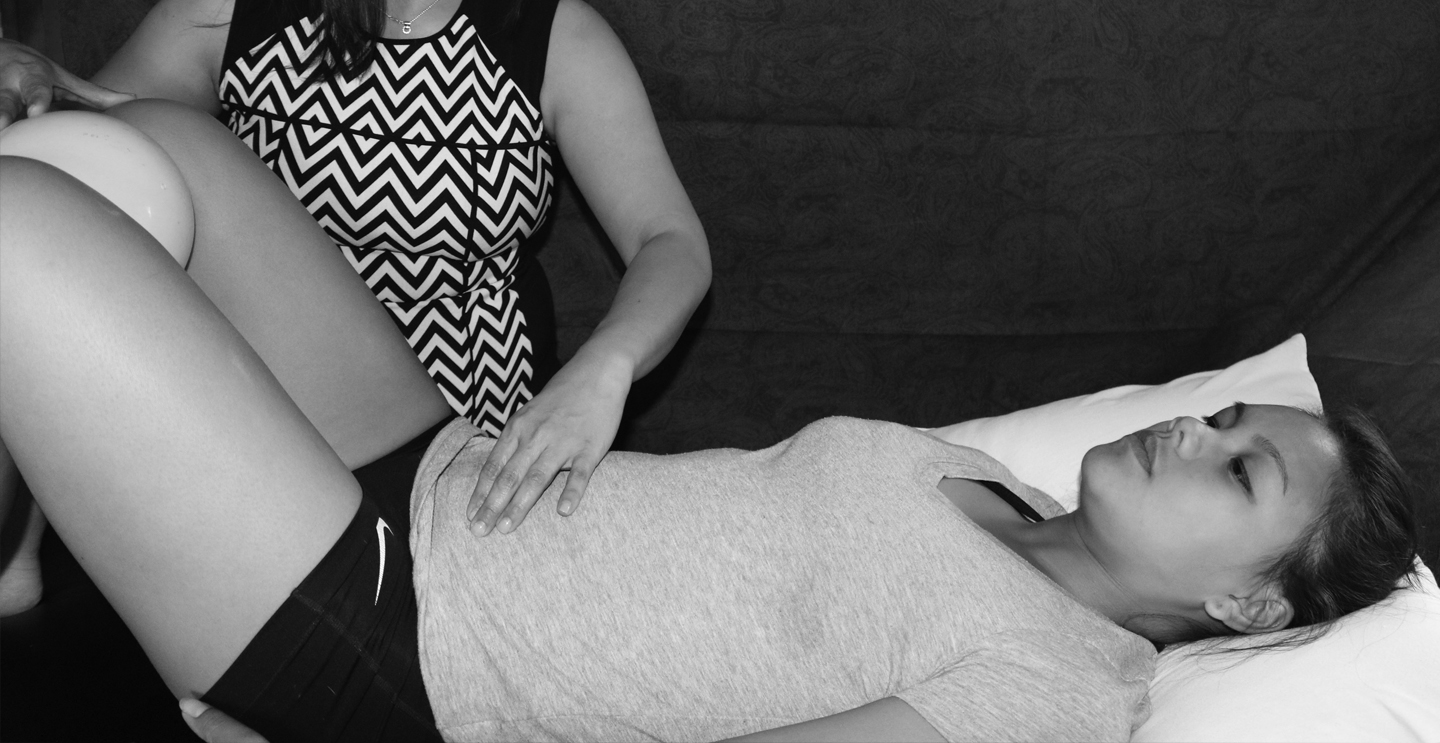
Pelvic floor muscles are a group of muscles that form a sling between the tailbone and the pubic bone. These muscles are involved in bladder and bowel control, provides support and stability to the spine and pelvis, and also plays a role in sexual functions.
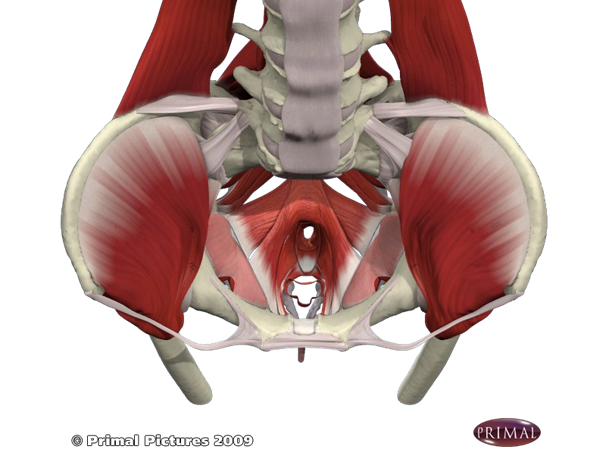
Pelvic Floor Dysfunction (PFD) refers to various conditions in which the pelvic floor muscle either becomes too tight or too loose which can lead to its inability to properly contract or relax. PFD may be accompanied by pain due to the development of trigger points within the pelvic floor muscle belly. These pelvic floor trigger points may result from postural alignment or biomechanical problems, connective tissue length/tension asymmetry, increased sympathethic activity, spine instability, sacro-iliac joint dysfunction, bladder/sphincter dysnergia, GI problems or other conditions related to urogynecological or gastrointestinal systems.
Common PFD Conditions
- Pelvic pain/sexual dysfunction (dyspareunia, vaginismus, vulvodynia, endometriosis, pudendal neuralgia)
- Urinary dysfunction (incontinence, overactive bladder syndrome, interstitial cystitis, prostatitis)
- Bowel dysfunction (constipation, fecal incontinence, irritable bowel dysfunction)
- Pelvic organ prolapse (bladder, uterus, rectum)
- Rectal pain syndrome (levator ani syndrome, coccydynia, proctalgia fugax)
- Post-surgical pain/adhesion (hysterectomy, cesarean section)
- Prenatal & post-natal musculoskeletal pain and dysfunction (diastesis recti, sacroiliac dysfunction, low back pain)
What to expect...
A comprehensive evaluation that may consist of:
- History of your symptoms
- Biomechanical assessment
- Range of motion and muscle testing
- Connective tissue and visceral mobility testing
- External observation of the perineum
- Sensory and reflex testing
- Biofeedback assessment of the pelvic floor muscles
- Internal assessment of the pelvic floor muscle to determine presence of trigger points and pelvic floor muscle strength, endurance and coordination
Our specially trained pelvic floor therapist will be able to determine any dysfunction in the muscles, connective tissue, bones and also abnormal recruitment patterns of the pelvic floor muscles. Treatment will be individualized and tailored to your needs and may include:
- Manual therapy (myofascial release, trigger point release, visceral mobilization, muscle energy techniques, connective tissue, scar, soft tissue and joint mobilization) to help release tight structures, improve mobility and decrease pain.
- Biofeedback training of the pelvic floor to help improve strength, endurance or the muscles’ ability to relax and coordinate its contraction.
- Education on proper alignment and body mechanics, relaxation techniques, management of symptoms and home exercise program.
- Other modalities for pain management (ice, heat, biofeedback, electric stimulation)